Pharmacology for Nursing Students
Dosage Forms & Routes of Drug Administration
Comprehensive study notes designed in Osmosis style to master pharmacological principles essential for safe nursing practice
Table of Contents
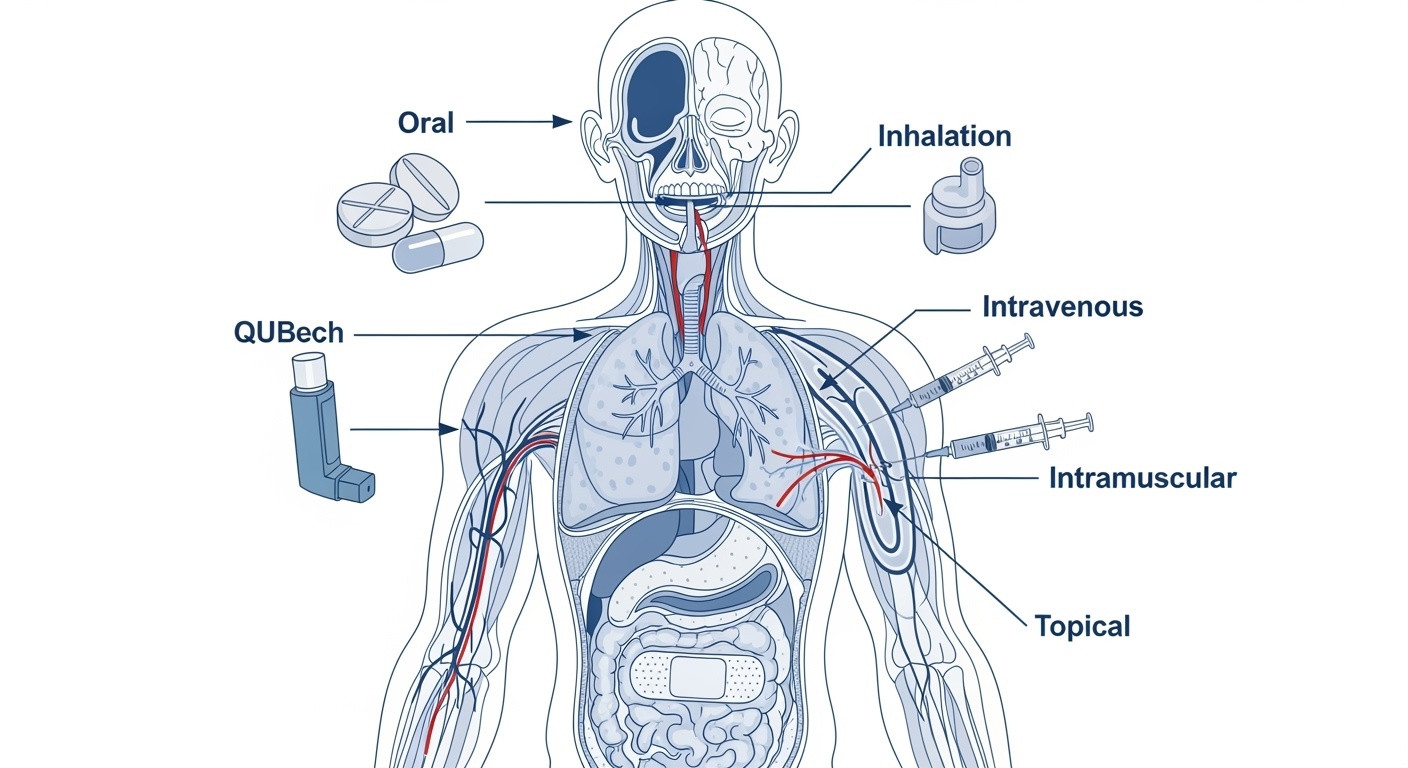
Comprehensive overview of drug administration routes and dosage forms
Introduction
Understanding dosage forms and routes of drug administration is fundamental to safe and effective nursing practice. This comprehensive guide explores the various ways medications can be formulated and delivered to patients, ensuring optimal therapeutic outcomes while minimizing adverse effects.
Learning Objectives
- Identify and classify different dosage forms
- Understand various routes of drug administration
- Apply pharmacological terminology in clinical practice
- Implement safe medication administration principles
- Recognize factors affecting drug absorption and distribution
The choice of dosage form and administration route significantly impacts drug bioavailability, onset of action, duration of effect, and patient compliance. As nursing professionals, we must understand these principles to provide safe, effective patient care and educate patients about their medications.
Pharmacology Terminology
Mastering pharmacological terminology is essential for effective communication in healthcare settings and safe medication administration.
Core Terms
What the body does to the drug (ADME: Absorption, Distribution, Metabolism, Excretion)
What the drug does to the body (mechanism of action, therapeutic effects)
Fraction of administered drug that reaches systemic circulation
Similar bioavailability and pharmacokinetic profiles between drug products
Memory Aid: ADME
Dosage Terms
- Dose: Amount of drug administered
- Dosage: Amount and frequency
- Therapeutic dose: Effective treatment amount
- Toxic dose: Harmful amount
- Lethal dose: Fatal amount
Response Terms
- Onset: Time to first effect
- Peak: Maximum effect time
- Duration: Length of action
- Half-life: Time for 50% elimination
- Steady state: Equilibrium level
Safety Terms
- Contraindication: Reason not to use
- Side effect: Unintended effect
- Adverse reaction: Harmful response
- Drug interaction: Effect modification
- Tolerance: Reduced response
Dosage Forms
Dosage forms are pharmaceutical preparations containing active pharmaceutical ingredients (APIs) in specific physical forms designed for optimal drug delivery and patient compliance.
Solid Dosage Forms
Tablets
- • Compressed solid dosage form
- • Various types: immediate, sustained, enteric-coated
- • Easy to manufacture and transport
- • Good stability and shelf life
Capsules
- • Hard or soft gelatin shells
- • Mask taste and odor
- • Easy to swallow
- • Can contain multiple drugs
Powders
- • Finely divided solid particles
- • Reconstituted before use
- • Suitable for unstable drugs
- • Pediatric formulations
Liquid Dosage Forms
Solutions
Homogeneous mixtures with drug completely dissolved
Suspensions
Dispersed solid particles in liquid medium
Syrups
Concentrated sugar solutions with medications
Emulsions
Dispersed immiscible liquids stabilized by emulsifiers
Semi-solid Dosage Forms
Ointments
- • Greasy, occlusive preparations
- • Oil-based systems
- • Prolonged contact time
- • Enhanced penetration
Creams
- • Oil-in-water emulsions
- • Non-greasy, easily absorbed
- • Cosmetically acceptable
- • Suitable for hairy areas
Gels
- • Semi-solid colloidal systems
- • Clear, non-greasy
- • Cooling effect on application
- • Good patient compliance
Memory Tip: S.L.S. Dosage Forms
Solid
Tablets, Capsules, Powders
Liquid
Solutions, Suspensions, Syrups
Semi-solid
Ointments, Creams, Gels
Routes of Drug Administration
The route of administration determines how a drug enters the body and significantly affects its absorption, distribution, onset, and duration of action.
Classification of Administration Routes
Enteral Routes
Enteral routes involve drug administration through the gastrointestinal tract. These routes are generally safer, more convenient, and more economical than parenteral routes.
Oral (PO)
Advantages:
- • Convenient and comfortable
- • Cost-effective
- • Self-administration possible
- • Reversible (induced vomiting)
Disadvantages:
- • First-pass metabolism
- • Variable absorption
- • Slow onset
- • GI irritation possible
Sublingual (SL)
Advantages:
- • Rapid absorption
- • Bypasses first-pass metabolism
- • Direct systemic circulation
- • Quick onset of action
Disadvantages:
- • Limited to small doses
- • Patient compliance issues
- • Taste considerations
- • Saliva dilution effects
Rectal (PR)
Advantages:
- • Useful when oral route unavailable
- • Partial bypass of first-pass
- • Local and systemic effects
- • Suitable for unconscious patients
Disadvantages:
- • Unpredictable absorption
- • Patient discomfort
- • Contraindicated in rectal disease
- • Limited social acceptance
Buccal
Advantages:
- • Rapid absorption
- • Avoids first-pass metabolism
- • Controlled release possible
- • Easy administration
Disadvantages:
- • Limited drug capacity
- • Taste and irritation issues
- • Eating/drinking restrictions
- • Accidental swallowing risk
Parenteral Routes
Parenteral routes bypass the gastrointestinal tract, providing rapid and predictable drug absorption. These routes require sterile preparations and proper injection techniques.
Intravenous (IV)
100% bioavailability
Direct entry into bloodstream
Best for:
- • Emergency situations
- • Large volume administration
- • Precise dosing requirements
Risks: Infection, embolism, phlebitis
Intramuscular (IM)
Moderate absorption rate
Dependent on muscle blood flow
Common sites:
- • Ventrogluteal (preferred)
- • Vastus lateralis
- • Deltoid (small volumes)
Max volume: 3mL adults, 1mL children
Subcutaneous (SC)
Slow, sustained absorption
Limited by blood supply
Ideal for:
- • Insulin administration
- • Heparin injections
- • Small volume drugs (<2mL)
Avoid irritating solutions
Intradermal (ID)
Minimal absorption
Local skin reaction
Primary uses:
- • Allergy testing
- • Tuberculin testing
- • Local anesthesia
Volume: 0.1-0.2mL maximum
Inhalation
Rapid systemic absorption
Large alveolar surface area
Delivery methods:
- • Metered-dose inhalers (MDI)
- • Dry powder inhalers (DPI)
- • Nebulizers
Requires proper technique
Intrathecal
Direct CNS access
Bypasses blood-brain barrier
Indications:
- • Spinal anesthesia
- • CNS infections
- • Cancer chemotherapy
High-risk procedure
Topical Routes
Topical routes provide local drug delivery with minimal systemic absorption, offering targeted therapy with reduced systemic side effects.
Dermal
- • Skin surface application
- • Local anti-inflammatory effects
- • Minimal systemic absorption
- • Creams, ointments, lotions
Ophthalmic
- • Eye drops and ointments
- • Precise dosing required
- • Sterile preparations
- • Limited contact time
Nasal
- • Local decongestant effects
- • Systemic hormone delivery
- • Rich vascular supply
- • Sprays and drops
Otic
- • Ear drops and solutions
- • Local antimicrobial therapy
- • Wax removal preparations
- • Temperature considerations
Memory Aid: E.P.T. Routes
Enteral
Through GI tract
- • Oral (PO)
- • Sublingual (SL)
- • Rectal (PR)
- • Buccal
Parenteral
Bypassing GI tract
- • Intravenous (IV)
- • Intramuscular (IM)
- • Subcutaneous (SC)
- • Intradermal (ID)
Topical
Local application
- • Dermal
- • Ophthalmic
- • Nasal
- • Otic
Nursing Considerations
Safe medication administration requires comprehensive assessment, proper technique, and continuous monitoring. Nurses play a crucial role in ensuring patient safety and therapeutic outcomes.
The Five Rights of Medication Administration
Right Patient
- • Two identifiers
- • Wristband verification
- • Ask patient to state name
Right Drug
- • Check medication label
- • Verify against order
- • Check expiration date
Right Dose
- • Calculate accurately
- • Double-check calculations
- • Use appropriate measuring devices
Right Route
- • Verify route in order
- • Assess route appropriateness
- • Use proper technique
Right Time
- • Follow scheduled times
- • Consider drug interactions
- • Account for meals
Pre-Administration Assessment
Patient Factors
Physical Assessment:
- • Vital signs
- • Weight and height
- • Organ function (liver, kidney)
- • Level of consciousness
- • Ability to swallow
Medical History:
- • Allergies and sensitivities
- • Current medications
- • Previous adverse reactions
- • Pregnancy status
Drug-Specific Factors
Pharmacokinetics:
- • Onset and peak times
- • Duration of action
- • Metabolism pathway
- • Excretion route
Special Considerations:
- • Food interactions
- • Storage requirements
- • Monitoring parameters
- • Contraindications
Route-Specific Techniques
Injection Techniques
IM Injection Steps:
- Select appropriate site and needle size
- Clean site with antiseptic
- Insert needle at 90° angle
- Aspirate to check for blood return
- Inject medication slowly
- Withdraw needle and apply pressure
Needle Selection Guide:
- IM: 1-1.5 inch, 21-23 gauge
- SC: 0.5-0.625 inch, 25-27 gauge
- ID: 0.25-0.5 inch, 26-27 gauge
IV Administration
IV Push Technique:
- Verify IV patency
- Check compatibility
- Administer at appropriate rate
- Flush line before and after
- Monitor for infiltration
Critical Monitoring:
- • IV site for signs of infiltration
- • Patient response to medication
- • Vital signs during administration
SAFE Medication Practice
Stop
Pause and focus before administration
Assess
Patient condition and medication appropriateness
Follow
Proper procedure and five rights
Evaluate
Patient response and document
Clinical Applications
Understanding practical applications of dosage forms and administration routes helps nurses make informed decisions in various clinical scenarios.
Emergency Situations
Cardiac Arrest
- Route: IV/IO preferred
- Rationale: Immediate systemic access
- Drugs: Epinephrine, atropine
- Alternative: Endotracheal if no IV access
Severe Allergic Reaction
- Route: IM (thigh)
- Rationale: Rapid absorption without IV
- Drug: Epinephrine auto-injector
- Site: Vastus lateralis muscle
Status Epilepticus
- Route: IV preferred, rectal alternative
- Rationale: Fast CNS penetration needed
- Drugs: Lorazepam, diazepam
- Consideration: Midazolam IM if no IV
Pediatric Considerations
Age-Appropriate Routes
- • IV: Scalp veins, foot veins
- • IM: Vastus lateralis preferred
- • Oral: Liquid formulations
- • Rectal: When oral not feasible
- • Oral: Flavored liquids, chewable tablets
- • IM: Vastus lateralis, ventrogluteal
- • Topical: Age-appropriate concentrations
- • Inhalation: With spacer devices
Special Considerations
- • Weight-based dosing (mg/kg)
- • Body surface area calculations
- • Maximum dose limitations
- • Age-specific pharmacokinetics
- • Immature metabolism
- • Different drug distribution
- • Higher risk of medication errors
- • Need for child-resistant packaging
Geriatric Applications
Physiological Changes
- Decreased gastric acid: Affects tablet dissolution
- Reduced muscle mass: Affects IM absorption
- Decreased renal function: Prolongs drug elimination
- Changes in skin: Affects topical absorption
Nursing Adaptations
- Swallowing assessment: Risk of aspiration
- Smaller needle gauge: Fragile veins
- Extended monitoring: Slower metabolism
- Polypharmacy concerns: Drug interactions
Safety Protocols and Error Prevention
Medication safety is paramount in nursing practice. Understanding common errors and implementing prevention strategies protects patients and ensures quality care.
Common Medication Errors
Dosage Errors
- • Calculation mistakes
- • Decimal point errors
- • Unit confusion (mg vs mcg)
- • Concentration errors
- • Pump programming errors
Double-check all calculations, use calculators, have colleague verify high-risk drugs
Route Errors
- • Wrong administration method
- • Inappropriate route selection
- • Tubing misconnections
- • Site selection errors
- • IV compatibility issues
Always verify route against order, use proper connectors, assess site appropriateness
Identification Errors
- • Wrong patient
- • Look-alike/sound-alike drugs
- • Similar packaging
- • Name confusion
- • Multiple patients in room
Use two patient identifiers, read labels carefully, separate similar medications
High-Alert Medications
PINCH Categories
Concentrated solutions, IV push
All formulations and concentrations
IV, transdermal, oral concentrates
All antineoplastic drugs
All routes and concentrations
Safety Protocols for High-Alert Drugs
Before Administration:
- • Independent double-check by two nurses
- • Verify calculation and dosing
- • Check patient parameters (labs, vitals)
- • Ensure proper monitoring equipment available
During Administration:
- • Use appropriate pumps with safety features
- • Continuous patient monitoring
- • Proper documentation
- • Have reversal agents readily available
Technology in Medication Safety
Electronic Systems
- Electronic Health Records (EHR)
- Computerized Provider Order Entry (CPOE)
- Electronic Medication Administration Record (eMAR)
- Clinical Decision Support Systems
Automated Dispensing
- Automated dispensing cabinets
- Unit-dose packaging systems
- Pharmacy robots
- Smart infusion pumps
Identification Technology
- Barcode medication administration
- RFID tracking systems
- Patient wristband scanning
- Medication verification systems
Culture of Safety
Individual Accountability:
- • Personal responsibility for patient safety
- • Continuous learning and competency maintenance
- • Speaking up when concerns arise
- • Following established protocols consistently
System Support:
- • Non-punitive error reporting systems
- • Regular safety education and updates
- • Adequate staffing and resources
- • Team-based approach to medication safety
Summary and Key Takeaways
This comprehensive review of dosage forms and routes of drug administration provides the foundation for safe, effective nursing practice in medication management.
Essential Knowledge
- Dosage forms (solid, liquid, semi-solid) each have specific advantages and applications
- Administration routes significantly affect drug bioavailability and patient outcomes
- Pharmacological terminology is essential for professional communication
- Patient assessment guides appropriate route and dosage form selection
Critical Skills
- Five Rights must be verified before every medication administration
- Proper technique for each administration route ensures safety and efficacy
- Error recognition and prevention strategies protect patients
- Special populations require adapted approaches and considerations
Continuing Education Recommendations
Stay Current:
- • New drug approvals and formulations
- • Updated safety guidelines
- • Technology advancements
- • Evidence-based practice changes
Practice Skills:
- • Regular competency assessments
- • Simulation-based training
- • Peer review and feedback
- • Case study discussions
Professional Development:
- • Pharmacology certification programs
- • Professional organization membership
- • Conference attendance
- • Research and quality improvement
Remember: Safe medication administration is not just a skill—it’s a commitment to patient safety and professional excellence.
Continue learning, stay vigilant, and always prioritize patient wellbeing in every medication decision.
